Fact-checked against Services Australia — Medicare on 2026-04-25.
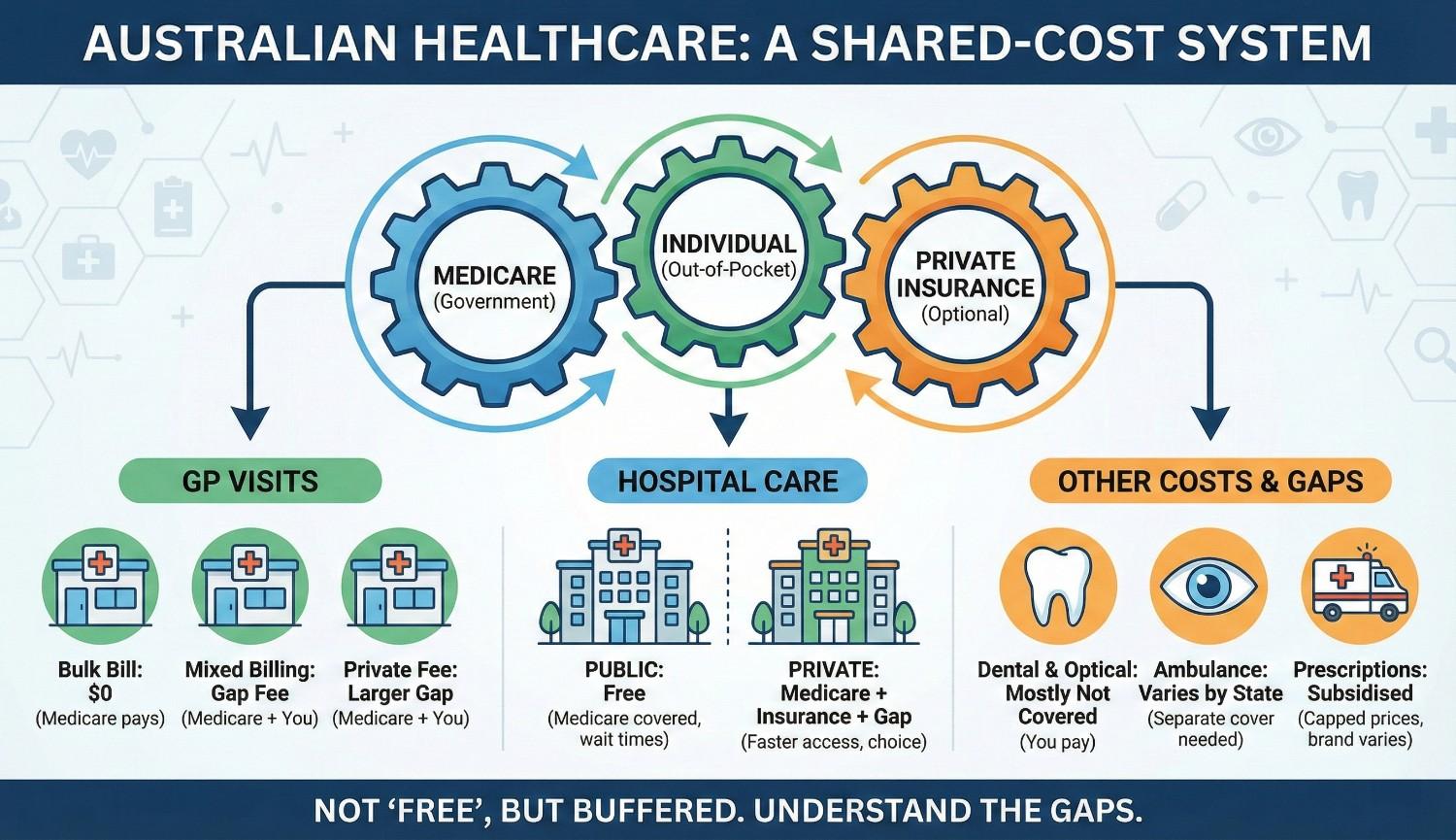
Healthcare in Australia is sometimes described as free, and sometimes described as surprisingly expensive. Both descriptions miss the actual structure. The thing is, healthcare costs in Australia run on layers — Medicare rebates, gap fees, the PBS, the Safety Net, and private insurance — and the price someone pays for any given service depends on which combination of layers applies. Essentially, “free” and “expensive” describe different patients in the same system. Anyway.
The four layers of healthcare costs
Bear with me. Almost every healthcare cost in Australia is shaped by a combination of four layers. Knowing which layer is doing what reduces a lot of confusion.
- Medicare rebates — the federal payment for medical services on the Medicare Benefits Schedule
- Provider fees — the amount the doctor, specialist, or clinic actually charges
- The PBS — federal subsidies for prescribed medicines on the Pharmaceutical Benefits Scheme list
- Private health insurance — optional cover that fills specific gaps the public system doesn’t
The structure of the broader system — public hospitals, the federal-state split, where private cover fits — is covered in our healthcare system structure explainer. This article is about the costs, specifically, that show up in real care.
Medicare rebates and the schedule fee
Quick framing. Medicare doesn’t pay a fixed dollar amount per visit. It pays a defined rebate per service, with each service identified by a Medicare Benefits Schedule (MBS) item number. A standard short GP consultation has one item number; a longer consultation has another; a specialist consultation has yet another. The Services Australia Medicare hub is the authoritative reference for how the rebate system works.
The MBS sets a “schedule fee” for each item. The Medicare rebate is a percentage of that schedule fee — typically 85% for out-of-hospital services and 75% for in-hospital private treatment. The patient or provider receives the rebate; the difference between the rebate and what the provider actually charges is where out-of-pocket costs sit.
In practice, this means two things matter for the cost of a service: the MBS item number (which sets the rebate) and the provider’s fee (which sets the total). Patients see the difference at the till.
Bulk-billing — what it’s and isn’t
Bulk-billing is the arrangement where a provider accepts the Medicare rebate as full payment for the service. The patient pays nothing at the time of the visit; the provider bills Medicare directly for the rebate amount.
The thing is, bulk-billing isn’t a discount — it’s a billing model. Providers who bulk-bill are accepting that the rebate is enough to cover the service. Providers who don’t bulk-bill have decided the rebate alone doesn’t cover their costs, so they charge the difference to the patient.
Bulk-billing rates vary substantially:
- Standard GP consultations are commonly bulk-billed for concession-card holders, less commonly for general patients (and the rates have shifted in recent years)
- Specialist consultations are rarely bulk-billed
- Many diagnostic services (pathology, simple imaging) are commonly bulk-billed
- Higher-complexity diagnostic services (MRI, certain scans) are often not
Knowing whether a provider bulk-bills before booking is the simplest way to avoid an unexpected fee. Reception staff usually answer this directly when asked.
Gap fees and out-of-pocket costs
A gap fee is the difference between what a non-bulk-billing provider charges and what Medicare rebates. If a GP charges $90 for a standard consultation and the Medicare rebate is around $42, the gap is roughly $48. The patient pays the full $90, then receives the rebate back (often instantly via electronic claiming).
Gap fees are common and legal. Providers set their own fees; Medicare doesn’t regulate them. The trade-off is patient choice: providers who set higher fees often offer shorter wait times, longer consultations, or specialist expertise that justifies the price for the patient.
For specialist consultations, gaps are usually higher. A first specialist consultation can have a gap of $100 to $200 or more depending on the specialty and location. The Services Australia Medicare Safety Net page covers what happens when these gaps add up over a year.
The Medicare Safety Net
The Medicare Safety Net is the federal mechanism that reduces out-of-pocket costs for patients who hit defined annual thresholds. It exists specifically because gap fees can stack up for people with chronic conditions, frequent specialist needs, or high-care families.
The Safety Net has two thresholds:
- Original Medicare Safety Net — once gap-fee spending hits the threshold, Medicare pays 100% of the schedule fee for further services (instead of 85%) for the rest of the calendar year
- Extended Medicare Safety Net — a higher threshold, after which Medicare pays a percentage of the gap above the schedule fee, capped at certain limits
Concession-card holders cross the thresholds at lower amounts. Families can register together so the spending is pooled.
Importantly, the Safety Net is automatic for individuals — Services Australia tracks the spending — but families need to register to pool. People who haven’t registered as a family often miss thresholds they would have crossed if pooled.
The PBS and prescription costs
The Pharmaceutical Benefits Scheme is the federal subsidy mechanism for prescribed medicines. The about-the-PBS page covers the listing process, the patient co-payment, and the safety net.
The way it works: medicines on the PBS list have a capped patient co-payment, with concessional rates for pension and healthcare card holders. Medicines not on the PBS are charged at full retail price unless covered by another scheme (like a private extras policy or a specific subsidy).
Three things affect prescription costs:
- Whether the medicine is on the PBS list — listed medicines have the capped co-payment; unlisted medicines don’t
- Whether the patient holds a concession card — pensioners and healthcare card holders pay much lower co-payments on PBS items
- Whether the PBS Safety Net has been hit — once annual PBS spending reaches the threshold, further medicines are free or near-free for the rest of the year
Patients on long-term medication often save substantial amounts each year by tracking PBS spending toward the safety net, and by asking the prescriber whether a PBS-listed alternative exists for medicines that would otherwise be at full retail price.
Private health insurance and the gap
Private health insurance in Australia is regulated at the federal level and runs alongside Medicare. The federal comparison portal at privatehealth.gov.au is the authoritative source for policy comparisons and the rules around the Medicare Levy Surcharge and Lifetime Health Cover loading.
What private cover changes about costs:
- Hospital cover — pays the difference between Medicare’s in-hospital rebate (75% of the schedule fee) and the actual cost of private hospital treatment, subject to policy limits
- Extras cover — subsidises dental, optical, physio, and other services Medicare doesn’t cover, up to annual limits
- Tax effects — some higher-income earners pay the Medicare Levy Surcharge if they don’t hold appropriate private hospital cover
What private cover doesn’t change:
- Standard out-of-hospital GP and specialist gap fees — these are still paid by the patient in most cases
- PBS prescription costs — these are governed by the federal PBS, not private insurance
- Public hospital treatment — eligible patients still get this free as public patients regardless of private cover
Eligibility for Medicare itself — the foundation that all of this sits on top of — is covered separately in our Medicare eligibility article.
Frequently asked questions
Why am I charged a gap fee at the doctor in Australia?
Gap fees happen when a provider charges more than the Medicare rebate amount. Medicare pays a fixed rebate per service (set by the Medicare Benefits Schedule); if the provider’s fee is higher, the difference is the patient’s out-of-pocket cost. Bulk-billing providers accept the rebate as full payment; non-bulk-billing providers pass on the difference. Right.
How does the Medicare Safety Net work?
The Medicare Safety Net reduces out-of-pocket costs once a patient or family hits an annual threshold. After the threshold is reached, Medicare pays a higher percentage of the schedule fee for out-of-hospital services for the rest of the calendar year. Two thresholds apply — original and extended — with concession-card holders crossing them at lower amounts.
Does private health insurance reduce gap fees?
It depends. Private hospital cover can reduce or eliminate gap fees for in-hospital private treatment, depending on the policy and the provider. Private extras cover subsidises out-of-hospital services like dental and physio that Medicare doesn’t cover. Neither type usually changes gap fees on standard Medicare-covered GP or specialist visits.
Where unexpected healthcare costs usually come from
Most unexpected healthcare costs in Australia don’t come from the obvious places. They come from three quieter ones: gap fees on specialist visits that turn out to be higher than the GP visits the patient was used to, prescriptions for medicines that aren’t on the PBS, and ambulance bills (which are state-level and not covered by Medicare). All three are technically published — the rules exist on .gov.au sites — but they aren’t the costs people generally expect.
The practical move, for someone managing healthcare costs over time, is to know which layer applies to which service: Medicare rebate for medical services, PBS for medicines, private cover for hospital and extras, state systems for ambulance. Asking about gap fees before booking, registering as a family for the Safety Net, and tracking PBS spending toward the safety net all reduce out-of-pocket costs over a year. None of these moves are individually large, but together they account for most of the difference between people who feel surprised by healthcare costs and people who don’t.